 
Unfortunately, atropine acts at the AV node and, as such, is rarely effective in raising the heart rate in patients with complete heart block. 
The initial management of bradycardic patients that are symptomatic usually begins with the use of intravenous atropine as per the advanced cardiac life support recommendations. A chest radiograph and complete blood count are necessary to evaluate for concomitant diseases. 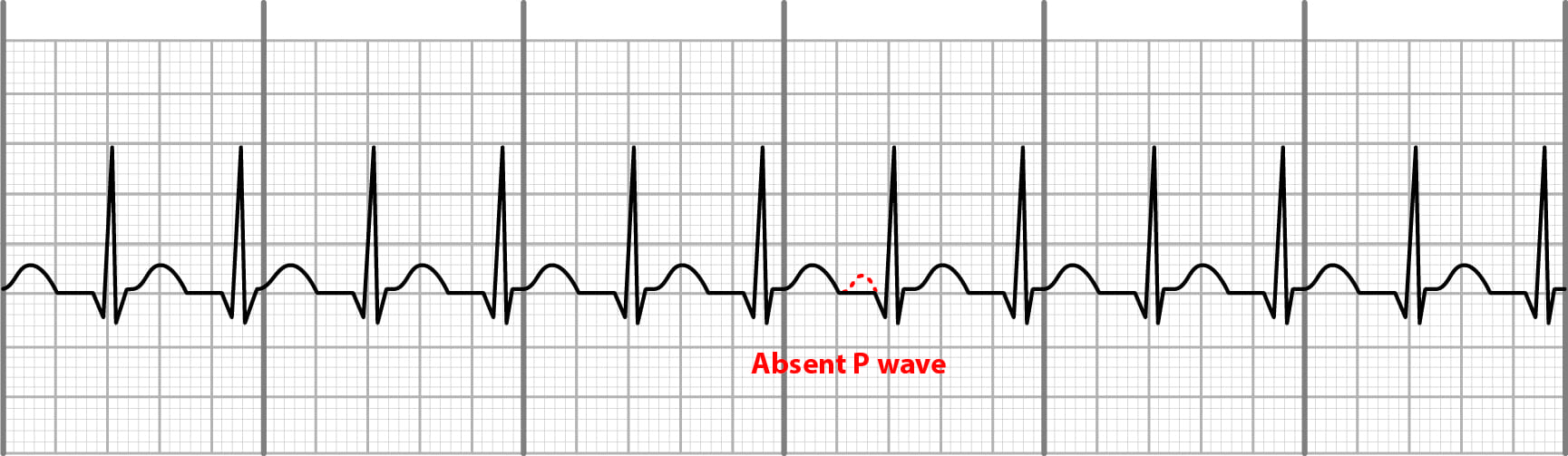
In patients who take digoxin, a digoxin level must be obtained to exclude digoxin toxicity. Troponin should also be evaluated and trended to check for myocardial infarction. A basic metabolic panel should be obtained to correct electrolyte abnormalities and to evaluate and correct the glucose, which might be low in beta-blocker toxicity. An ECG should also have an evaluation for signs of ischemia. Depending on the location of the block, the QRS complex might be a narrow morphology (junctional escape QRS complex) or a wide morphology (ventricular escape QRS complex). The atrial rate, demonstrated by the P wave, should be faster than the ventricular rate, as demonstrated by the QRS complex. The electrocardiogram will have completely independent atrial and ventricular activity with no relation between the P wave and the QRS complex. After stabilizing the patient, the most important component of the evaluation is the electrocardiogram. Patients with complete heart block might present in significant distress. If there is coexistent heart failure evidenced by S gallop, peripheral edema, or hepatomegaly, then immediate pacing is a crucial part of management.Īttention should be paid to any signs of infection or skin rashes, such as rheumatic fever, Lyme disease, and endocarditis, which cause heart blocks. The presence of any new murmurs should be noted as a strong association exists between complete AV block and cardiomyopathies, mitral calcification, aortic calcification, or endocarditis. Especially with heart rates below 40/min, patients might also present with features consistent with decompensated heart failure, respiratory distress, and hypoprofusion, such as diaphoresis, tachypnea, altered mental status, retraction, cool skin, and decreased capillary refill. Thus a very large pressure wave is felt up against the vein. The physical exam is usually remarkable for bradycardia. JVP examination often demonstrates cannon A-waves owing to the simultaneous contraction of the atria and ventricles. The past medical history will often include the presence of cardiovascular disease and/or its risk factors, including diabetes mellitus, hypertension, dyslipidemia, smoking, etc. Patients with complete AV-block accompanying an acute myocardial infarction often have ischemic symptoms of chest pain or dyspnea. The patient's status at the time of presentation can vary depending on the concurrent disease and the rate of the escape rhythm. They may have significant hemodynamic instability and can be obtunded. Usually, they may present with generalized fatigue, tiredness, chest pain, shortness of breath, presyncope, or syncope. Patients with third-degree blocks can have varying clinical presentations. This rhythm is unresponsive to atropine and exercise. The heart rate will typically be less than 45 to 50 beats/min, and most patients will be hemodynamically unstable. The SA node continues its activity at a set rhythm, but the ventricles activate through an escape rhythm that can be mediated by either the AV node (junctional escape), one of the fascicles (fascicular escape), or by ventricular myocytes themselves (ventricular escape rhythm). As the name implies, no impulses from the SA node get conducted to the ventricles, leading to a complete atrioventricular dissociation. The third-degree block is also known as complete heart block. These delays present in the form of AV blocks, which are of first, second, and third-degree. When there is a pathological delay in the AV nodal conduction, it is visualized on an electrocardiogram as an alteration in the PR interval. From the AV node, the electrical impulse passes through the His-Purkinje system to activate ventricular contraction. That impulse gets delayed in the AV node, assuring the contraction cycle in the atria is complete before a contraction begins in the ventricles. Under its regular function, the AV node receives an impulse from the SA node. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
